Suicide: How NYU’s Campus Crisis Response Is Failing Students and Staff
The author is a native New Yorker and a recent alumna of NYU. Currently involved in clinical research, she plans to pursue a career in nursing and public health.
Interior of Elmer Holmes Bobst Library lined with aluminum panels.
June 4, 2018
Note from the editor: Names have been omitted from this op-ed for the privacy of those mentioned. WSN independently fact-checked the content of this op-ed.
The NYU Student Health Center states its mission is to “Enhance the health and well-being of students in support of their learning and success.” Its services were expanded when the university created the Wellness Exchange in response to numerous suicides that took place publicly during the academic year from 2003 to 2004. The Wellness Exchange prides itself on being an award-winning resource for student health, and certainly, many people have benefitted from its services. However, several students have reported troubling encounters, and despite the significant resources allocated for this purpose, NYU has since continued to have many incidences of student and staff suicides, with at least three confirmed suicides in the past two months alone. Here, I will candidly share my own experience, as one lens through which to explore the critical issue of crisis response at NYU.
* * *
In my final year of college, during an excruciatingly tense medical appointment, a Primary Care practitioner communicated to me their own depression, the futility of counseling and off-handedly mentioned suicide. Over the course of the following month, I related the incident to several SHC staff, in person and over the phone, but was consistently met with skepticism. Some counselors suggested I had misunderstood the incident due to stress, and no one expressed any intention to act on my concern. A Psychology fellow dismissed my thoughts as “catastrophic thinking;” in his clinical notes in my electronic health record, he diagnosed me as severely depressed, characterizing me as someone who probably suicidal. Bizarrely, I was never made aware of this black mark on my medical record. While the professionals sat idly by, the practitioner who had sparked my concern left their position at the end of the semester and went to a tragic, untimely death.
At the time, I was a financially self-supporting student, with a lapse in health insurance coverage, facing medical, financial and personal barriers, for which I sought help. One Wellness clinician casually suggested that I find a therapist, although they couldn’t provide me with a single affordable referral. During an unrelated medical follow-up, a nurse assumed my Urgent Care visit from the previous semester must have been for psychiatric reasons when it was actually due to pyelonephritis. Yet another SHC employee asked if I had attempted suicide. These assumptions – all made by providers who had never previously interacted with me – raised red flags that my medical records were potentially falsified with misinformation.
Concerned about this situation, I repeatedly emailed the Wellness Exchange, only to be persistently ignored by the same counselors who had previously rushed to invalidate me. Next, I emailed [email protected] and the nonchalant response was along the lines of, ‘thanks for letting us know,’ as if I were a restaurant patron complaining about a shortage of napkins. I reached out to a patient advocate about my falsified medical records; however, he seemed apathetic and never followed up. The SHC executive director dodged my emails. After I reported my experience to the Office of Compliance and Risk Management, I eventually received a phone call from NYU’s assistant director of Wellness & Crisis Response. For a crisis responder, she didn’t seem concerned with urgency: by the time she called me, I had already left NYU and was working as an HIV counselor. Over the phone, it became evident that she had not read the report, nor was she even aware of her colleague’s death, or my concerns about my records, which she never looked at. Nevertheless, she coldly insisted no investigation was needed. She did not bother to look at any of the evidence readily available: an obituary in The New York Times, electronic records of staff interactions and even a phone recording between myself and a Wellness staff member.
How could a group of well-educated professionals collectively make such a mistake in judgment?
Perhaps it was not the fault of individuals, but the result of a system in which clinicians are expected to perform like robots, and patients are reduced to an intake number. In the many times I reached out for help at the SHC, I put my faith in its providers, who serve integral roles within the university. The Wellness Exchange previously won an award for “An Innovative Approach to Address Mental Health on Campus.” Yet to my dismay, most clinicians never even asked me relevant questions about myself to gather information. Instead, they stared intently at their clipboards and computer screens, mindlessly reciting the same scripted statements, checking off boxes and regurgitating the same misconceptions – as they likely had been trained to do.
When challenges become too overwhelming, we are continually told to seek help — but when I sought help, my thoughts were dismissed and concerns carelessly tossed aside. In healthcare we are taught to “Do No Harm”, but I left NYU more harmed as a result of interactions with SHC personnel than had I not reached out in the first place. While I persisted and advocated for myself, I couldn’t pretend this didn’t adversely impact me, both academically and in terms of my wellbeing. Here, I would be remiss not to mention I was genuinely grateful for the assistance I did receive from the Moses Center for Students With Disabilities, without which I may not have graduated.
* * *
In reaching out to administrators many times to resolve these issues — Student Affairs Vice President Marc Wais, CAS Deans Gene Jarrett and Richard Kalb, Health Executive Dr. Carlo Ciotoli and multiple staff within the SHC — I was consistently ignored. Actions speak louder than words, and their silence is deafening. To me, it is painfully obvious that NYU students and alumni burden ourselves with tremendous student debt to fund the salaries and vacation homes of executives who do not seem to care about our lives. Additionally, considering how common campus shootings, which often end in suicide, have become in the United States, perhaps the university should reconsider how it responds to students reporting crisis concerns, as a step to prevent further incidents. It is time to become less reactive and more proactive.
To combat student suicides, NYU originally installed eight-foot-high polycarbonate barriers along the balconies of the Elmer Holmes Bobst Library. Nevertheless, determined students leaped to their deaths. Subsequently, NYU installed plexiglass barriers, and when that failed, aluminum screens were created. Public perception is the primary concern: NYU builds impressively visible barriers, but when students quietly take their lives, or end up sexually assaulted, traumatized or depressed, we are left to sink or swim in a sea of apathy. To add to the stigma, students are typically not notified about suicide, with the exception of deaths that take place in a public setting. Unfortunately, I learned this when one of my own roommates at NYU, who openly struggled for years, took her own life shortly after graduation, and it was not made known by the university.
It is up to students to demand better because while the executives stubbornly stick their heads in the sand, nothing will change. As I embark on my own career in healthcare, these facts and tragedies remain at the forefront of my mind. I carry my experiences with me always, a constant reminder to treat people with respect, dignity, to extend compassion, and to always advocate for patients where no one stood up to advocate for me.
Wellness Director, Zoe Ragouzeos, Ph.D., has declined to comment.





























































































































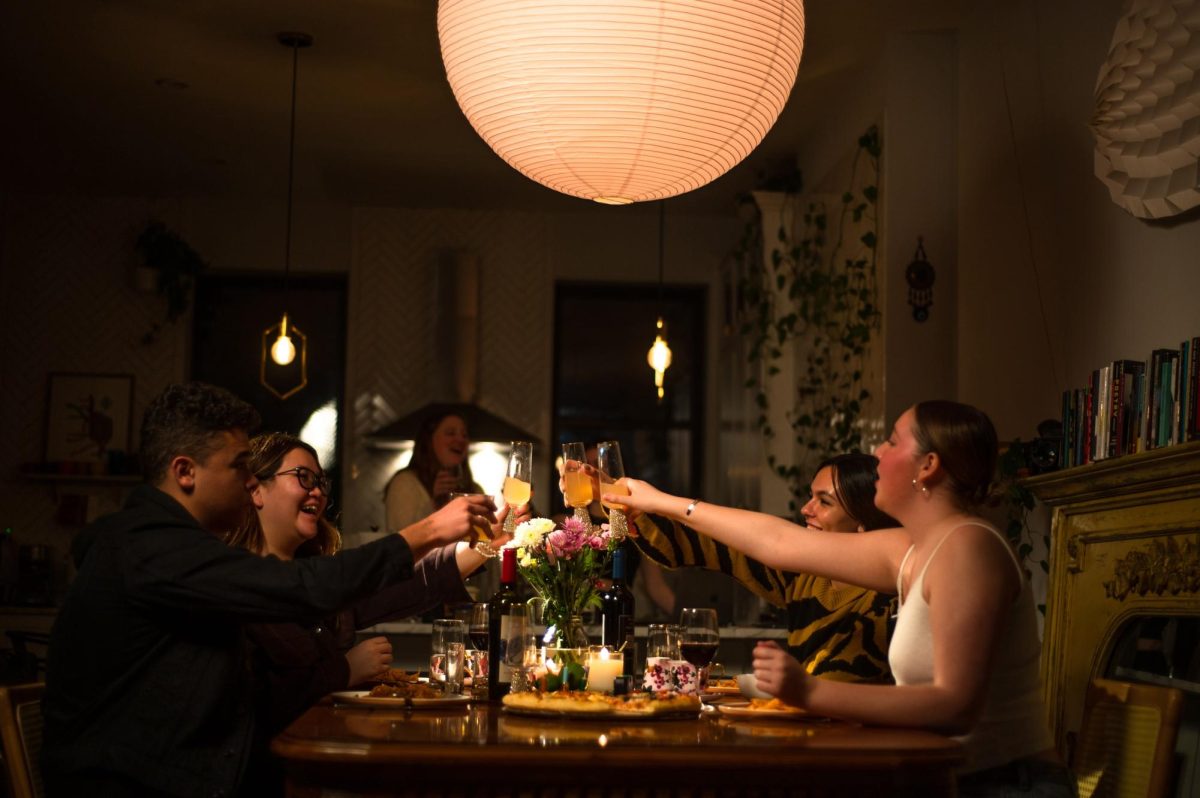
















one who knows • Jun 9, 2018 at 4:45 pm
i can relate a lot to what has been written here. The wellness exchange is not so organized despite the good intent of particular (not all) therapists. The problem is with the system itself, and the most concerning issue is that they do not have any valid or relevant referrals for students who need long term treatment.
maedchenhaft • Jun 6, 2018 at 4:31 am
Thanks a lot for the post.Really thank you! Much obliged.
Darcey Pittman • Jun 5, 2018 at 5:04 pm
Such a well done piece. Thank you for sharing your experiences. Mental health services at the college level, and especially at an intense university like NYU, need to be discussed more instead of swept under the rug.